Tenting Skin – It takes a long time for the skin to return to normal or to “repair” itself during an examination. This may indicate severe dehydration, which requires immediate treatment. In addition, you have a reduced skin turgor and cannot increase your fluid intake (e. g. due to vomiting). Skin turgor is also a sign of fluid loss (dehydration). Diarrhea or vomiting may result in fluid loss. Babies and infants with these conditions can quickly lose a lot of fluid if they don’t drink enough water. Fever accelerates this process.
To check the turgor of the skin, the doctor uses the skin between two fingers to lift it. It is usually contained in the forearm or abdomen. The skin is held for a few seconds and then released. Skin with normal turgor quickly returns to its normal position. Skin with low turgor takes time to return to its routine work.
It is deficient in reasonable to plain fluid loss. Mild dehydration happens when the fluid loss is 5 % of body weight. Sensible dehydration is 10 % loss, and essential thirst is 15 % or more body weight loss. Hence, edema is an illness in which unsolidified matter accumulates in the tissues and causes swelling. This makes it extremely difficult to pinch the skin.
What Is a Skin Tenting Fracture?
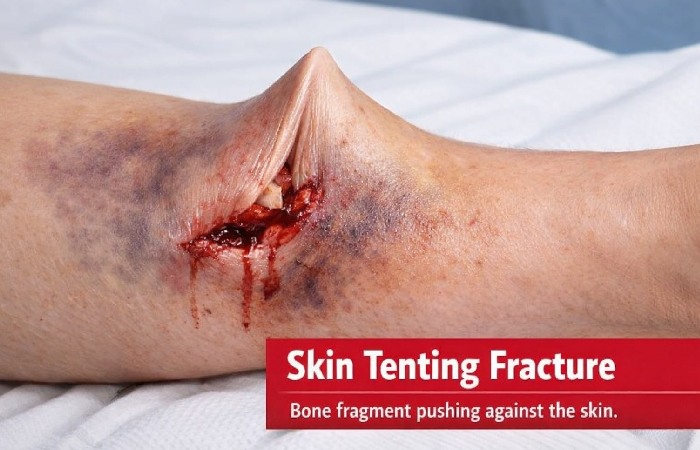
A skin-tenting fracture refers to a type of bone break where the broken bone pushes in contradiction to the skin from beneath, causing the skin to stretch firmly over the fracture site, like a “tent.” This is frequently seen in fractures of long bones, such as the tibia (shin bone).
The overstretched skin is at high risk of tearing, which can turn a closed break into an open fracture if not conserved promptly. Skin bivouacking in fractures is considered a medical emergency because it can compromise blood flow, increase the risk of contagion, and delay healing. Immediate medical attention is required to realign the bone and relieve pressure on the skin properly.
What Does Tenting Skin Mean?
It takes a long time for the skin to return to normal or for the skin to “repair” itself during an examination. This may indicate severe dehydration, which requires immediate treatment. In addition, you have a reduced skin turgor and cannot increase your fluid intake (e. g. due to vomiting).
Reduced skin turgor is indicate if the skin (on the back of the hand in an adult or on the abdomen in a child) is stretch for a few seconds and does not return to its original state. Poor skin turgor is causes by desiccation. In addition, because of not drinking enough water and several other things can lead to dehydration, including vomiting. Diarrhea.
How Does Dehydration Cause Tenting Skin?
The more hydrated you are then the more elastic your skin becomes and recovers immediately after you tweak it. Conversely, if you are dehydrated, the skin loses its elasticity, and it takes a while to return to normal, and the more likely it is to build up.”
| Step | What Happens in the Body | Effect on the Skin |
| 1 | The body loses too much fluid through sweating, illness, or low water intake. | Skin cells begin to lose moisture. |
| 2 | Edited body fluids decrease the skin’s natural springiness | Skin becomes dry and less flexible |
| 3 | The layer under the skin (subcutaneous tissue) loses hydration | Skin construction weakens |
| 4 | When the skin is gently stretched or pulled, it cannot quickly return to its original position. | The skin stays raised or “tented.” |
| 5 | This delayed return is known as skin tenting, a sign often associated with thirst. | Designates the body needs fluids |
When Does Tenting Skin Indicate a Medical Problem?

Tenting skin is often a sign of thirst or reduced skin elasticity, but in some cases, it can indicate an underlying medical issue that needs attention. While infrequent mild tenting may happen in older adults due to natural aging, tenacious or severe tenting, especially when accompanied by other symptoms, should be assessed by a healthcare expert.
Severe Dehydration: Caused by extreme vomiting, diarrhea, fever, or inadequate fluid intake.
Electrolyte Imbalance: Low levels of sodium, potassium, or other electrolytes disrupt fluid balance.
Malnutrition: A lack of protein or essential nutrients weakens the skin’s structure.
Chronic Illnesses: Situations such as diabetes, kidney disease, or heart failure can decrease skin hydration and elasticity.
Shock or Blood Loss: Abridged flow may cause rapid loss of skin turgor.
Burns or Severe Skin Conditions: Injury to skin layers can mimic or worsen tenting.
How To Improve the Tenting Skin?
Improving tenting skin usually refers to enhancing skin elasticity and firmness, especially if the skin “tents” when pinched—a sign of aging, dehydration, or loss of collagen. Here’s a detailed guide:
Hydrate Your Skin
- Drink at least 8 glasses of water daily.
- Use a moisturizer with hyaluronic acid or glycerin to retain skin moisture.
- Apply hydrating serums regularly.
Boost Collagen Production
- Topical retinoids (retinol, tretinoin) stimulate collagen and improve elasticity.
- Vitamin C serums help with collagen synthesis and antioxidant protection.
- Peptide creams also support skin structure.
Food Sources:
- Bone broth, fish, eggs, citrus fruits, berries, and leafy greens.
Protect Against Sun Damage
- Use broad-spectrum sunscreen (SPF 30+) daily, even indoors.
- Wear protective clothing and avoid prolonged sun exposure.
- Sun damage accelerates loss of elasticity and collagen.
Exercise Your Skin
- Facial exercises can strengthen underlying muscles and support firm skin.
- Neck and jawline exercises may help improve loose skin appearance.
Consider Professional Treatments
- Microneedling: Stimulates collagen production.
- Radiofrequency therapy: Tightens skin and improves elasticity.
- Laser treatments: Help with skin rejuvenation.
- Fillers: In cases of significant sagging, dermal fillers restore volume and smoothness.
Healthy Lifestyle Choices
- Quit smoking: Smoking damages collagen and elastin.
- Limit alcohol: Excessive alcohol dehydrates and weakens skin.
- Sleep well: 7–9 hours supports skin repair.
- Balanced diet: High in antioxidants, proteins, and healthy fats (omega‑3).
Avoid Rapid Weight Changes
- Rapid weight loss or gain can worsen skin tenting. Aim for gradual weight changes to allow skin to adapt.
Symptoms Associated with Tenting Skin

| Symptom | Description | Possible Cause / Notes |
| Behind Skin Return | Skin stays raised when pinched in its place of breaking back | Specifies abridged skin elasticity, often due to dehydration |
| Dry Skin | Skin feels rough, flaky, or less supple | Common with fluid loss or malnutrition |
| Sunken Eyes | Eyes appear hollow or sunken | Frequently occurs alongside simple thirst |
| Fatigue / Weakness | Feeling tired or weak | Related to fluid and electrolyte imbalance |
| Low Blood Pressure / Dizziness | May feel dizzy when standing up | Sign of important fluid loss |
| Rapid Heart Rate | The heart may beat faster than normal | The body compensates for low fluid volume |
| Dark Urine / Low Urine Output | Urine develops focused or less frequent | Marker of thirst |
| Dry Mouth / Thirst | Determined thirst and dry oral cavity | Early cane of fluid loss |
Risk Factors for Developing Tenting Skin
Tenting skin occurs when the skin loses its normal liveliness, often due to dehydration or serious health issues. Convincing evidence indicates that certain factors increase the probability of developing this disorder, making it important to be aware of them, especially in vulnerable individuals.
Insufficient Fluid Intake: Not drinking enough water frequently can reduce skin hydration.
Excessive Fluid Loss: Vomiting, diarrhea, sweat, or fever can quickly reduce body fluids.
Advanced Age: Elderly individuals naturally have reduced collagen and skin energy.
Malnutrition: The absence of protein, vitamins, and minerals damages skin formation.
Chronic Illnesses: Conditions such as Diabetes, kidney disease, or heart disease can damage hydration and skin health.
Extreme Heat or Cold Exposure: Ecological stress can increase watery loss or dry out the skin.
Medications: Some diuretics or laxatives may increase thirst if not managed properly.
What is the Difference Between Skin Turgor and Tenting ?

| Feature | Skin Turgor | Tenting Skin |
| Definition | The skin’s aptitude to return to its normal state after being tense | A disorder where the stressed skin stays lifted and does not quickly return to its usual position |
| Indicates | Normal hydration and skin bounciness | Thirst or loss of skin elasticity |
| Skin Response | Strained skin snaps back immediately | Strained skin leftovers “tented” or raised |
| Cause | Well, hydrous skin with normal collagen | Fluid loss, undernourishment, aging, or certain diseases |
| Clinical Use | Used to measure hydration status in patients | Used as a sign of dehydration or decreased skin elasticity |
| Observation | Normal in all age groups if hydrous | More marked in older adults or severely dry persons |
Treatment Options for Tenting Skin
| Treatment Option | Description | When It’s Used / Notes |
| Oral Fluids | Eating water or electrolyte solutions to rehydrate the body | Mild to moderate dehydration |
| Intravenous (IV) Fluids | Organization of saline or electrolyte fluids directly into a vein | Severe dehydration or inability to take fluids orally |
| Balanced Diet / Nutrition | Irresistible protein, vitamins, and minerals to support skin health | Malnutrition-related skin tenting |
| Moisturizers / Skin Care | Using balms to hydrate dry skin | Helps improve skin bounciness temporarily |
| Treatment of Underlying Conditions | Managing diseases like Diabetes, food issues, or heart problems | Speeches are the root cause of fluid imbalance or poor skin health |
| Nursing Vital Signs | Sprawling blood pressure, heart rate, and urine output | Safeguards hydration treatment is actual |
| Emergency Care for Fractures | For skin tenting due to fractures, bone reform, and coiled care | Prevents skin failure and contagion. |
Common Causes for Tenting Skin
Tenting skin occurs once the skin loses its normal bounciness and does not quickly return to its original position after being stretched. The most common cause is Dehydration, but numerous other medical or ecological issues can also contribute. Once the form lacks sufficient fluids or nutrients, the skin becomes less flexible and may show this camping result.
Dehydration: Loss of body fluids from sweating, vomiting, looseness, or not drinking adequate water.
Severe Weight Loss: Loss of subcutaneous fat reduces skin support.
Malnutrition: A lack of vital nutrients weakens skin structure and its bounce.
Aging: Natural aging reduces collagen and skin elasticity.
Prolonged Illness: Chronic conditions such as Diabetes or Cholera can lead to fluid inequity.
Excessive Heat Exposure: High fevers may lead to heavy sweating and fluid loss.
Prevention Tips to Avoid Tenting Skin

Tenting skin is primarily caused by dehydration and reduced skin elasticity. Averting it includes maintaining proper hydration, a balanced diet, and overall skin health. Regular monitoring and healthy habits can significantly reduce the risk.
Stay Hydrated: Drink plenty of water throughout the day, especially in hot weather or when you’re ill.
Use Oral Rehydration Solutions (ORS) When Wanted: Helps replace lost electrolytes during diarrhea, vomiting, or heavy perspiration.
Eat a Balanced Diet: Include protein, vitamins (A, C, E), and minerals to support skin elasticity.
Moisturize Often: Keep skin hydrated with creams, oils, or natural creams like coconut oil.
Monitor Fluid Loss: Watch for signs of dehydration, such as dry mouth, fatigue, or dark urine.
Manage Chronic Situations: Properly control diseases such as diabetes or kidney disorders that affect hydration.
Avoid Excessive Heat or Sun Exposure: Protect skin from dehydration due to high fevers.
Regular Check-ups: Ageing and at-risk persons should have routine health monitoring to catch early signs of thirst.
Price of Treatment for Tanning Skin in India
Here’s an overview of projected treatment costs for treating skin-related thirst and its management in India (2026 estimates):
| Treatment / Service | Approximate Cost in India (INR) | Notes |
| Oral Rehydration Solution (ORS) sachets | ₹3 – ₹10 per sachet (₹15 – ₹30 for multi‑pack) | Very reasonable & widely available at drugstores. (search.everythingbranded.com) |
| Basic dehydration management (clinic visit / OPD) | ₹500 – ₹5,000 | Includes doctor conversation & simple rehydration care. |
| Venous (IV) fluids (hospital/clinic) | ₹1,000 – ₹3,500 (outpatient) | Cost includes fluids, consumables & basic nursing; may vary by city and facility. |
| IV fluids + electrolyte correction | ₹2,500 – ₹8,000+ | For reasonable to severe dehydration requiring treatment care. |
| At‑home IV hydration facilities | ₹500 – ₹3,000+ | Mobile IV drip/home brew (fluid + setup + nurse/technician). |
| Hospital fee for severe thirst | ₹5,000 – ₹15,000+ | Fee + IV therapy + remark; cost varies significantly between secluded and group facilities. Revealing |
Price in India, UK, USA, and London Of Treatment Costs for Tanning Skin
Here’s a contrast table of estimated treatment costs for encampment‑skin-connected dehydration/rehydration care (such as ORS and IV hydration) in India, the UK, the USA, and London (UK), based on typical valuing sources (2026 estimates):
| Treatment / Service | India (INR) | UK (GBP) | London (GBP) | USA (USD) |
| ORS sachet (single) | ₹3 – ₹20 per sachet | ~£1 – £2 (estimated retail) | ~£1 – £3 (central London) | ~$1 – $3 (retail) |
| Basic clinic consultation for dehydration | ₹500 – ₹5,000 | £50 – £150 (GP/private) | £60 – £180 (private) | $100 – $300 (urgent care) |
| IV hydration (clinic/outpatient) | ₹1,000 – ₹8,000 per session | £100 – £200* | ~£150 – £280+ per session | $75 – $400 per session |
| Emergency room IV hydration (severe) | ₹3,000+ (hospital; varies) | NHS A&E free (tax-funded) | NHS A&E free (tax-funded) | $500 – $1,000+ (ER billing) |
| IV fluids + electrolytes (improved therapy) | ₹2,500 – ₹8,000 | £150 – £300* | ~£150 – £300+ | $100 – $500+ |
Procedure for Homecare – Tenting Skin
You can quickly check at home whether you are dehydrate. First, squeeze the skin on the back of the hand, abdomen, or front of the chest under the collarbone. This shows the turgor of the skin.
Mild desiccation takes some time to return to normal skin. To rehydrate, drink more liquid, especially water. A strong turgor indicates moderate to severe fluid loss. Please get in touch with your provider immediately. It is also called Doughy skin; Poor skin turgor; Good skin turgor; Decrease skin turgor.
- Poor skin turgor occurs with vomiting, diarrhea, or fever.
- The skin returns to its normal state very slowly, or it “stretches” during a check-up. This can indicate severe dehydration that needs to be treated quickly.
- You have decreased skin turgor and cannot increase your fluid intake (e.g., because of vomiting).
Conclusion
In my content, I want to state that tenting skin naturally drops some of its ability to stretch and recover as it grows. Solar radiation and habits such as smoking can accelerate this process. There are many successful treatments to improve skin elasticity. Lifestyle changes, such as wearing sunscreens, can help slow them down and minimize their impact.

